Masks are all but gone in my neck of the woods. A couple stores have employees that wear them, but not many, and then very few customers do. The people I know who don't wear masks seem to fall in three camps: The first are people with kids who are beyond their control (too young to be non-conforming mask wearers or rebellious teens), and they're absolutely terrified to the point of having to convince themselves, "We're all going to die of something!" in order to sleep at night. To them, wearing a mask is admitting to themselves that there's something to fear, and that's just not something their psyche can take right now. The second are people who have had a mild version with no lasting effects and are certain, based on their own experience, seeing it with their own eyes, that it's not a big deal. And the third group are people who watch very different media than I follow, and they are very convinced that the pandemic ended. Didn't I get the memo?? They really believe I'm crazy to keep wearing a mask now that it's all over. I might believe them - I'd love for it to be true - if it weren't for so many scientific journal articles that say otherwise.
It ain't over.
Two CBC articles posted just today make that abundantly clear. Mike Crawley reported on an emergency room crisis in which patients are waiting an average of 20 hours, and up to 48 hours, in ER before getting a bed in a ward:
"Patients in emergency rooms around Ontario are waiting record lengths of time to get admitted . . . at a time of year when the burden on emergency departments usually eases. . . . Key factors driving the long wait times are largely spin-off effects of the pandemic: High rates of staff calling in sick or unable to work because they've been exposed to COVID*-19. Patients whose illnesses are more severe, often because they delayed seeking treatment during the big pandemic waves. . . . The ratios of patients to staff are growing dramatically. . . . The acuity or the sickness level of our patients is far higher than it has ever been."
Peggy Lam wrote about the months-long waiting times in LongCovid treatment centres.
"Demand is so high that patients getting referrals now have to wait until November to get their first appointment. . . . Doctors across the country are starting to see increased volumes of requests for referrals for these specialized clinics. . . . [Dr. Neeja Bakshi looks] at both pharmacotherapy (medicines), rehab, allied health, anything that we think that will help this patient. . . . One of the things I'm seeing in the majority of my patients is a high heart rate or something called POTS (postural orthostatic tachycardia syndrome). . . . We need more clinics, we need more places that people can go with these multidisciplinary care teams to support them, and those clinics need funding. . . . . [Susan Thiele says] Just walking like five feet was exhausting. I could hardly do it. . . . One sip of soup and then I'd have to rest and try to recover and catch my breath again to take another one. . . . There was still no recommended treatment for her symptoms, other than simply rest."
In Canada, about 10% have contracted Covid, and a low estimate of 10% of people will get LongCovid (many places suggest 20-30% is more realistic), which means at least 1% of our population. So, about one in every hundred people in every city in Canada is dealing with this right now. That translates to, so far, about 12 kids in my school affected with extreme fatigue, difficulty breathing, brain fog, pain, stomach problems, or organ failure - unless we got lucky (and someone else bears the mean brunt of our luck). A friend of mine lamented being almost the only teacher at his school to still wear a mask. Our schools aren't safe, and our luck won't last forever:
Some people still think it's no worse than the flu. As ICU doctor WesEly explains, survivors of the flu don't complain of 200 long-term symptoms. The differences can be seen in animal studies as well, which validate patient claims since, "Rodents won't 'dream up' symptoms or tissue changes." Animals (and humans) behave differently after having it:
"Chronic inflammation in the olfactory system affects our emotional, sensory, and brain function (cognition). . . . The olfactory bulb is directly connected to the limbic system. Smell is connected to emotion and memory! This would explain, even when the virus is long gone, problems in LongCovid patients' ability to heal fully from newly minted brain fog and mental health disorders. . . . If the brain is abnormal, we'd expect its cellular metabolism to be diseased as well. Sadly, it is. These clusters of PET-proven hypometabolism in different brain regions matter on a human level. They are associated with more numerous functional complaints and symptoms of ongoing problems with smell, memory/cognitive disabilities, chronic pain, and sleep disorders. Brain PET studies in other LongCovid patients showed hypometabolism (think hibernating) in areas explaining problems with smell, fatigue, etc. The authors write this supports a hypothesis of post-viral, persistent systemic inflammation. Neuropsychiatric manifestations more frequently seen in LongCovid include depression, anxiety, PTSD, sleep disturbances, fatigue, and debilitating cognitive deficits."
"Living with it" to some people means letting everyone get infected, arguing that it's bound to happen anyway. But that defeatist view ignores potential leaps in vaccine production and policy changes that could further reduce transmission. The longer we can go without getting it, the better chance we'll have of better treatment. And we know how to reduce transmission: JUST WEAR A MASK! Surgical masks will only protect other people from your exhalations, but wearing an N95 and glasses/goggles will protect YOU from getting it or bringing it home.
Jon Parsons, author of COVID-19 and Ethics in Canada: The Failure of Common Decency, recently wrote about the psychology behind living with it:
"The 'learning to live with it' phase of the pandemic functions through widespread denial of the reality of ongoing harm. That denial is paradoxically enabled by a basic tendency toward optimism, which although a positive trait gets in the way of effective action. Lauren Berlant calls this 'cruel optimism,' in the sense that the desire to always look on the bright side stops people from recognizing the harms being done to them, or doing anything to address those harms. The tendency is to believe 'everything will work out for the best.' For example, mass infection means exposing young people to the virus over and over again. While parents may intellectually realize the risk, the intellectual realization is suppressed by the overwhelming need to believe their children are happy, healthy, and have bright futures. Likewise, people may intellectually know there are significant risks from infection, not just of hospitalization and severe outcomes but also risks associated with long covid. The optimistic impulse encourages them to believe it can't happen to them -- until, that is, it does.
On the broader social level, there is an optimistic tendency to believe in grand narratives of overcoming. Good inevitably triumphs and the righteous prevail. In their day-to-day lives, people are obliged to act happy-busy-good, and to do otherwise is to be labelled a malcontent. Optimism is a positive trait in many ways. It can help us see the best in others and to strive to achieve great things, even in the face of adversity. But it is also something that can enable enormous harm when it functions as a mechanism of denial. To say optimism as it relates to the pandemic is cruel is not a call for pessimism, but rather for a hard-nosed realism. It is a call for a clear recognition of the enormous harm being done, followed by reasonable and readily available measures to stop unchecked mass infection. As it relates to the current stage of the pandemic, optimism is getting in the way of many people recognizing the harm to themselves, their loved ones, and their communities. And it is getting in the way of doing anything to stop those harms."
We need ways to wake us up to this hard-nosed realism. Maybe we need to see some TikToks from friends and relatives of this 1%, seeing the specific effects of the illness, before we'll start to react to the pending threat! The BA.4/5 wave looks to be just starting and really hitting us late summer or early fall. In South Africa, the death rate is over three times current Covid-19 death rates. We can prepare for this. Or not. I hope the powers that be have the wherewithal to institute mask mandates again, but I won't hold my breath! We know what to do, AND we've done this type of thing before with Spanish flu and cholera. But maybe the problem now is that our ability to tackle this type of thing as a unified team was only possible before neoliberal politics and privatization of healthcare and such blatant greed and polarization in politics. I'm not sure we still have that "can do" attitude necessary to take a hard look at reality and act.
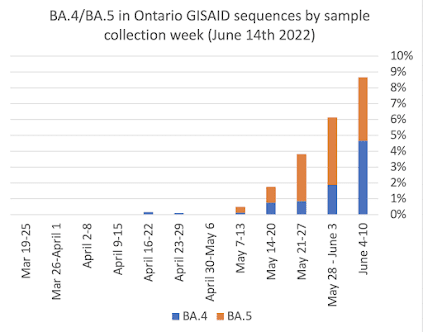
ETA: Almost 9% of Ontario cases are now BA.4/5. They're heeerre. And increasing by 40% each week!
Some who get LongCovid can recover. This 9-minute video by Stanford neurologist Michelle Monje explains how even mild or asymptomatic infections have long-term consequences, but she also explains that it's possible to re-set the cells in LongCovid patients the way people are able to recover from brain fog after getting chemo - but sometimes up to a year after. She also adds that she's "not at all ready to decrease mitigation efforts. We need to not fatigue of these efforts as difficult as they are." Elsewhere many people from all walks suggest that the best LongCovid prevention if you do get covid is rest. That doesn't just mean to stop working a bit, but to actually convalesce, to stop doing anything but sit outdoors watching the birds, bundled in a blanket, like in the old tuberculosis sanitariums, for three months, but I don't have any studies to back that up. And we've already seen how hard it is to act preventatively with just a mask on in public. I'm not sure many would be able to shut down their lives briefly in order to save themselves when the odds are in their favour with at least a 70% change of not getting LongCovid. The question of the day is: Is it worth the risk?
*Style note: I don't understand writing "COVID" in all caps when it's not an acronym. I understand SARS-CoV-2, which is an acronym (severe acute respiratory syndrome corona virus 2), but "covid" is a portmanteau of corona and virus, so shouldn't it just be "covid"? Curious.

No comments:
Post a Comment